Claim/Line Check or Remittance Date is Required on Adjudicated Claims. 2320/2430.DTP*573
|
Rejection Message Claim/Line Check or Remittance Date is required on adjudicated claims. 2320/2430.DTP*573 |
|
|
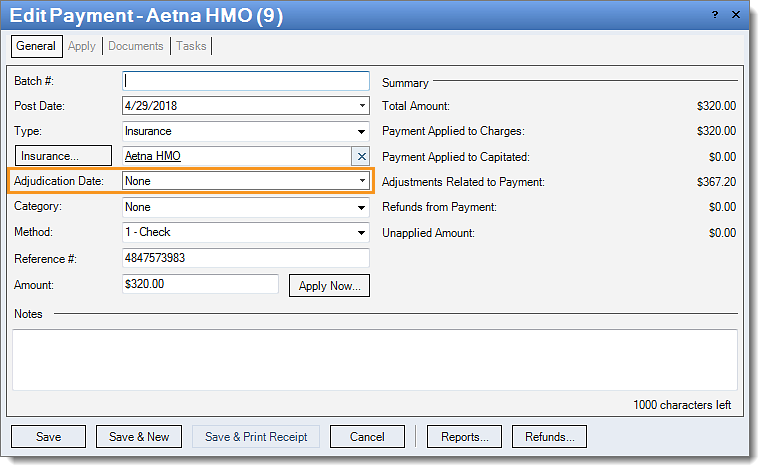
Rejection Details This rejection indicates the adjudication date is missing on the payment from the primary payer. |
|
|
Resolution Follow the instructions below to add an adjudication date to the primary payment:
Then, rebill and resubmit all affected claims. |
|